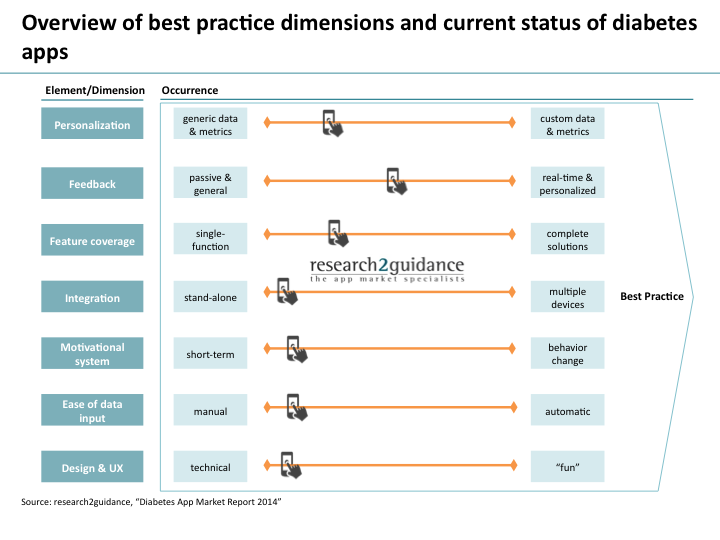
Today’s diabetes apps are far away from meeting the seven best practice standards
Mobile apps that support diabetics raise huge expectations but fall short of meeting best practice standards, which results in a low prevalence.
This is one of the results of our latest study on the mHealth app market: “Diabetes App Market Report 2014”.
The mHealth Economics 2017 Report is out.
Download the report for free!
Mobile apps can support the daily management of diabetes by supporting behavior changes, facilitating communication and easing the hassle of keeping track of all relevant parameters that have an influence on the disease. However, only a few apps utilize their potential. Most of the apps are too narrow in their functionality or too technical. To become a daily companion, diabetes apps must be individualized and fun to work with. They have to make life easier especially by automating the collection and sharing of data.
A 26 year old woman with type one diabetes expresses their experience with current diabetes apps.
“I tried different apps to have an easier life, but the problem always was, that they were only another form of my notations.”
In the 5th year of the app episode, it is astonishing that the majority of diabetes apps do not comply with standards that are widely accepted in the rest of the app market.
These app standard could be translated into 7 best practice elements a diabetes app should take care of.
These elements represent concepts and functionalities, which contribute to the success of a diabetes mobile application. By applying these best practice elements, mobile apps would come closer to leverage the potential they have in better supporting diabetes management.
1) Personalization: A successful diabetes app should allow the user to choose how data is displayed, how and what information is transmitted to third parties (such as family, friends, physicians, social networks), what metrics are being measured and what are the optimal levels for these metrics, taking into account various lifestyle factors. Personalization also means that diabetes apps should provide active feedback and actions to improve behavior based on the data generated by users.
2) Feedback: In order to sustain behavioral change, successful diabetes apps should include a social dimension and create a supportive network (family, friends, HCPs) to provide real-time feedback and coaching. Successful diabetes apps are encouraging sustained usage by giving users information and feedback on their progress.
3) Feature coverage: In order to simplify the self-management of diabetes apps, which address users with this condition should include all the tools and features that are needed for successfully keeping diabetes under control.
4) Integration and interoperability: Diabetes apps, just like mHealth apps in general, should be designed in a way that allows users to input and access their data through multiple devices from various sources. Ideally, diabetes apps would be integrated with external devices, sensors, databases and other apps, which help users achieve better control of critical health parameters in the management of diabetes (such as blood glucose levels, blood pressure, cholesterol), support the necessary lifestyle changes (weight management, exercise, nutrition) and provide new ways for connecting patients with their physicians (electronic health records). Integration gives access to a unified view on the patients’ health status and diabetes management, making it easier to identify trends, possible improvements and provide high-level personalized feedback. This also facilitates the integration of diabetes apps in the patients’ daily live and the result is simplified use and monitoring, as well as increased acceptance.
5) Motivational system: A good diabetes app should include a well-designed motivational system, which engages users, provides incentives for constant use and ultimately leads to behavior change. Best practice apps make full use of gamification elements.
6) Ease of data input: The usage should be effortless. Diabetes apps should fit seamlessly into users’ lives and routines, making the input of data as easy as possible without requiring too much effort from the users. Solutions should automatically transmit their glucose readings, for instance, from the blood glucose monitor to the mobile device.
7) Design & user experience: The aesthetic dimension plays a very important part in keeping users engaged and motivated and, at the same time, it can constitute a powerful differentiation element. Just like with any other app, the design and initial visual impression determines the entire user experience and can definitely determine whether a diabetes app is successful or not.
Most diabetes apps available today either do not make use of these best practice elements or they include such functionalities at their most basic level.
A user of diabetes apps summarizes the weaknesses of today’s diabetes apps.
“The intentions behind the apps I’ve seen are great, but in practice they quickly lose their luster. If an app isn’t integrated into something I already do or use quite often, or isn’t very simple [not time-consuming], I’ll abandon it. I don’t want to log in to another website; I don’t want to go somewhere I’m not already at – which, social-media wise, is going to Facebook. What I want is something that makes my life easier rather than cause me grief when I forget to check in or enter the info, and it shouldn’t take longer to load an app and do what I need with it than it does to open a notebook and use a pencil.”
However, there are also applications which aim to deliver complete solutions for the management of diabetes and they include sophisticated features that facilitate and encourage user acceptance and adaption. We will shortly publish an interview with one of the founders of mySugr, a diabetes app that demonstrates how a fresh design and gamification elements can drive usage up. Please come back soon.
For more information about the “Diabetes App Market 2014” report click here.
Your feedback on diabetes apps and their best practice elements are highly welcome.